Fusion
Sacroiliac Joint Fusion
(MIS and Posterior/Lateral)
Stabilizing the SI joint so you can move confidently again.
When the sacroiliac (SI) joint becomes arthritic or unstable, it can cause deep low-back, buttock, groin, or leg pain that mimics sciatica. If focused conservative care fails, minimally invasive sacroiliac joint fusion can stop the painful micromotion and restore stability. At Desert Spine and Pain in Phoenix, neurosurgeon Dr. David L. Greenwald, M.D., FAANS, FACS performs SI fusion through posterior and lateral MIS approaches, selecting the route that best fits your anatomy and goals. We pair precise diagnosis with a calm, step-by-step plan so surgery feels understandable—not intimidating.

Over 100 5-Star Reviews!

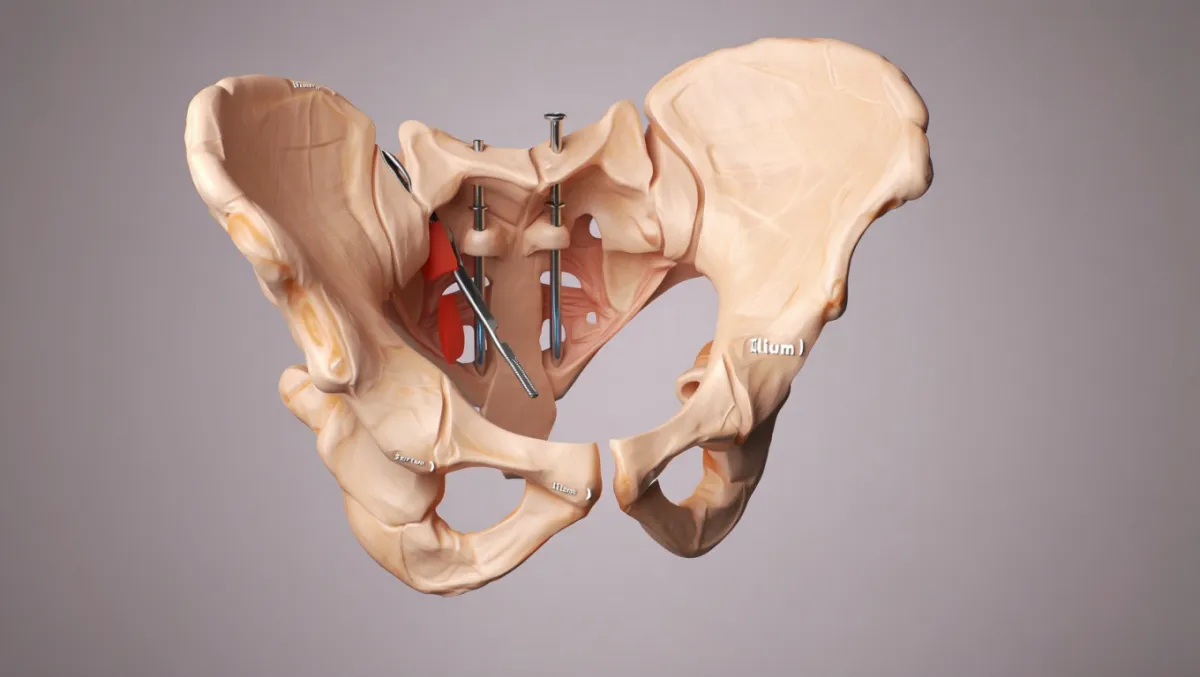
When SI Fusion Is Considered (and when it isn’t)
Good candidates typically have:
Pain localized over the posterior superior iliac spine (one finger-breadth below the dimple), often worse with standing, stairs, or rolling in bed
Multiple positive SI provocation tests on exam (e.g., FABER, Gaenslen, Fortin finger)
Clear relief after a diagnostic SI joint injection (strong confirmation the SI joint is the pain generator)
Persistent pain despite Physical Therapy, Medications, activity modification, and Bracing
Not ideal when pain arises primarily from lumbar disc/stenosis, hip pathology, generalized pain syndromes, active infection, or uncontrolled medical issues. We’ll rule out mimickers and often coordinate care if multiple sources coexist.
Want a deeper dive on the condition itself? See Sacroiliac Degeneration.
Imaging & Diagnostic Pathway
X-rays (pelvis, inlet/outlet views) to evaluate joint alignment and hardware if any.
MRI/CT to assess degeneration, exclude fractures or tumor, and understand bony corridors.
Diagnostic SI injection (local anesthetic ± steroid). Significant temporary pain relief confirms the joint as the culprit and predicts good surgical response.
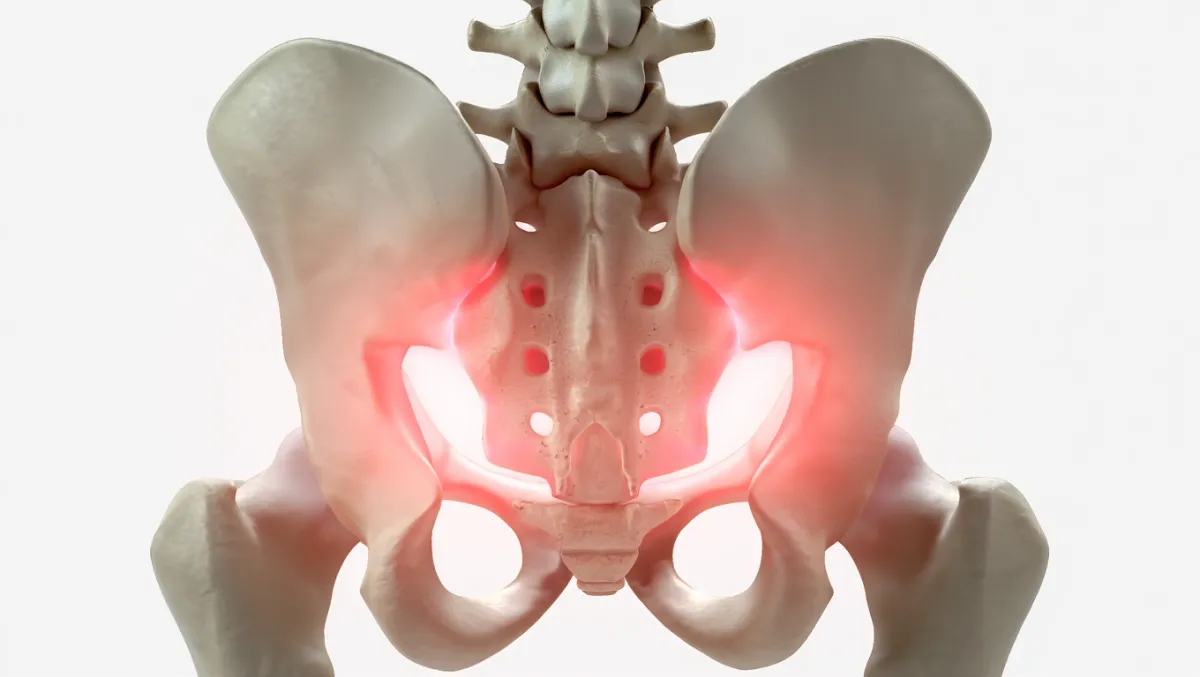
Approaches We Offer (and why)
We tailor the approach to your anatomy, prior surgeries, and goals:
MIS Lateral (Trans-iliac to Sacrum) Fusion
Side-entry through a small lateral buttock/flank incision. Implants traverse the SI joint from the ilium into the sacrum with fluoroscopic guidance. Excellent immediate stability; restores load-sharing across a broad footprint.
Best when: you have favorable pelvic anatomy and we want robust, multi-implant fixation.
MIS Posterior (Posterior/Posterolateral) Fusion
One or two small posterior incisions. We access the dorsal joint or the posterior intra-articular cleft to place graft/implants or transfixation devices.
Best when: lateral corridor is limited by body habitus/iliac crest or when posterior pain generators and anatomy favor a direct posterior route.
Both are minimally invasive, typically outpatient or 23-hour stay, and avoid large muscle dissection of open historical techniques.
How to Prepare (no surprises)
Stop nicotine (it hinders bone healing/fusion).
Review blood thinners/NSAIDs timing with us.
Optimize diabetes, nutrition, and bone health.
Set up a “recovery zone” at home (firm chair with arms, clear walk paths, shower chair if needed).
Line up a ride and a helper for 24–48 hours.
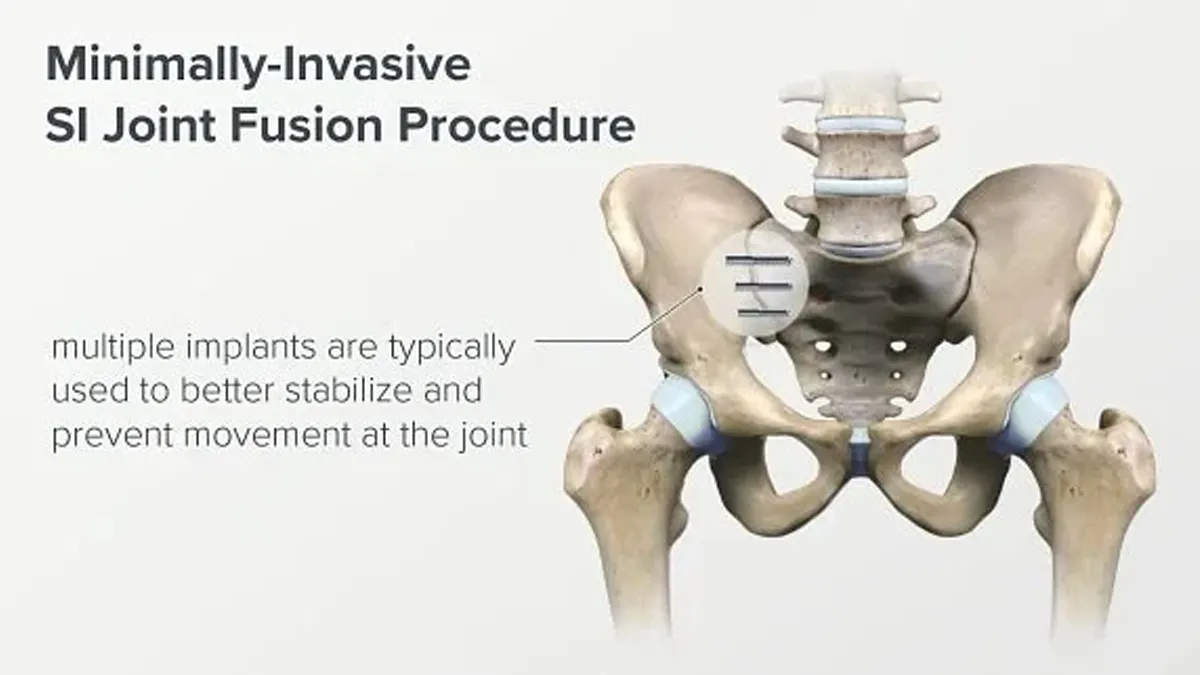
The Procedures Explained
Simply Explained
MIS Lateral SI Fusion
Positioning: On your side.
Tiny incision: 2–3 cm over the lateral buttock/iliac bone.
Live X-ray guidance: We map safe paths through the ilium across the SI joint into the sacrum.
Joint preparation: We create a channel and roughen (decorticate) bone to encourage fusion.
Implants placed: Usually 2–3 implants are inserted across the joint to lock out painful motion.
Close & recover: Small bandage; you stand and walk with help the same day.
MIS Posterior SI Fusion
Positioning: On your stomach with soft chest/pelvic pads for comfort.
Tiny midline or paramedian incision(s): 1–2 cm.
Target the joint posteriorly: A working cannula reaches the posterior SI joint or its cleft.
Decortication & graft/implant: We pack bone graft and place a posterior implant or transfixation device to stabilize the joint.
Close & recover: Small dressing; same-day mobilization.
Going home
Most patients leave the same day or the next morning with simple wound care, a walking plan, and a clear follow-up schedule.
Surgeon-level detail (for those who want the full picture)
MIS Lateral
Position: True lateral decubitus; AP/inlet/outlet fluoroscopy used throughout.
Trajectory planning: Guidewire from ilium → across SI joint → sacral ala/body; avoid neural foramina and anterior sacral cortex.
Channel creation: Cannulated drill/burr over guidewire creates the path; decortication optimizes osteointegration.
Implants: 2–3 porous or fenestrated transiliac-to-sacrum implants sized under fluoro; alignment verified on AP/inlet/outlet.
Adjuncts: Local autograft/allograft chips placed as indicated.
Closure: Layered absorbable sutures; no drain in routine cases.
MIS Posterior/Posterolateral
Position: Prone on radiolucent table; AP/outlet fluoro for sacral landmarks.
Access: Small posterior incision to dorsal SI joint; working cannula docked.
Preparation: Decortication of dorsal/posterior intra-articular surfaces; curettage of synovium as needed.
Fusion construct: Dorsal implant and/or interpositional allograft packed into the joint; optional trans-articular screw or dedicated posterior device per anatomy.
Final check: Stability confirmed; hemostasis and layered closure.
Implants, Graft Choices, and Why They Matter
Implants: Titanium or porous-coated devices designed to encourage bone on-growth/in-growth and resist micromotion.
Bone graft: Local autograft + allograft (and, in select patients, cellular allograft) supports fusion biology.
Number of implants: Typically 2–3 across the joint laterally; posterior systems often combine graft + a single implant depending on construct.
Benefits You Can Expect
Small incisions, less soft-tissue disruption → typically less pain and faster recovery
Immediate mechanical stability with modern implants
High patient satisfaction when diagnosis is confirmed by injection response
Often outpatient with walking the same day
Risks & How We Reduce Them
All surgeries carry risk, but we work methodically to reduce each one:
Infection/bleeding: Antibiotics, meticulous sterile technique, and tiny incisions.
Implant malposition or nerve irritation: Real-time fluoroscopy (AP/inlet/outlet), careful trajectories, and an experienced neurosurgical team.
Non-union (no fusion): Strict nicotine cessation, appropriate grafting, and follow-up imaging.
Persistent pain from another source: We confirm the diagnosis with exam + diagnostic injection and address coexisting lumbar/hip issues.
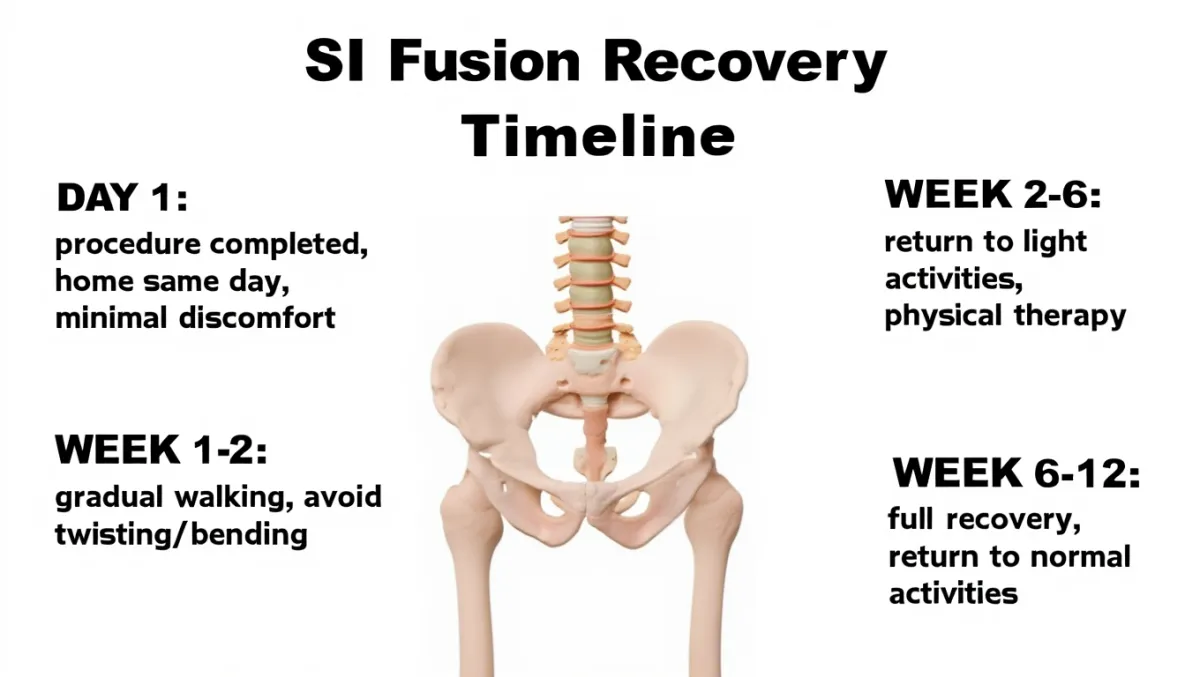
Recovery Timeline (typical pattern)
Day 0–1: Stand and walk with assistance; home same day or next morning.
Weeks 1–2: Short, frequent walks; keep incision clean/dry; avoid deep bending/twisting and heavy lifting.
Weeks 2–6: Most return to desk work; progressive walking program.
6–12 weeks: Begin or advance PT for hip/core strength and gait; activity widens.
3–6 months: Ongoing strengthening; many resume low-impact sports and heavier household tasks.
6–12 months: Fusion consolidation confirmed on X-rays/CT as indicated.
We use multimodal pain control (acetaminophen ± NSAID if appropriate, brief muscle relaxer/nerve-modulator, and lowest necessary short-course opioid). See Medications.
Life After SI Fusion
The SI joint normally moves very little, so fusing it does not reduce meaningful flexibility.
Most patients report easier transitions (sit↔stand, stairs, rolling in bed) and improved walking tolerance.
We’ll guide a return-to-work plan tailored to your job—office roles often by 2–4 weeks; heavier roles take longer.
How We Decide Between Lateral and Posterior MIS
We consider:
Pelvic shape & corridor size (iliac crest height, sacral orientation)
Prior surgeries/implants and scar patterns
Pain location & exam findings (dorsal vs deep intra-articular tenderness)
Your overall goals and need for bilateral vs unilateral fusion
We’ll show you your images and explain—clearly—which route gives the safest, strongest result for you.
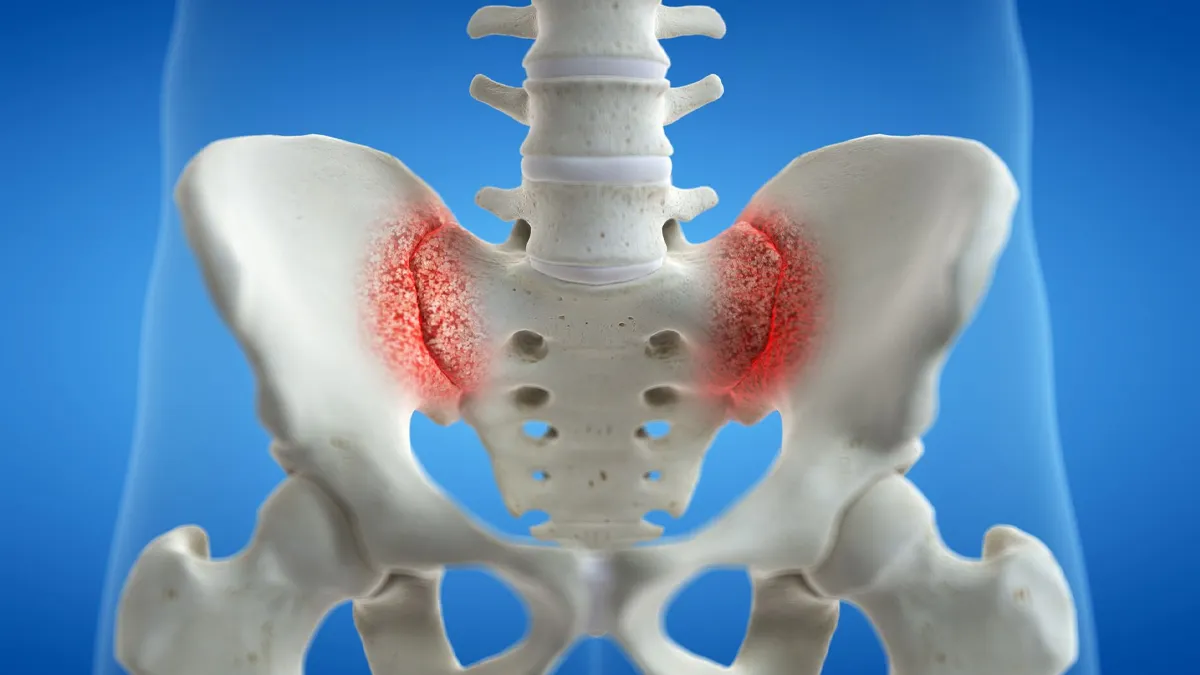
Why Choose Desert Spine and Pain?
Premier Phoenix center with a neurosurgeon-led team focused on precision MIS techniques
Diagnostic rigor (exam + imaging + confirmatory injection) so surgery is reserved for the right problem
Compassionate coaching before and after surgery, with Physical Therapy integrated at the right time
A full spectrum of options—from conservative care to advanced MIS fusion—so your plan is personalized, not one-size-fits-all
Frequently Asked Questions
How do you confirm my pain is really from the SI joint?
We combine exam maneuvers with imaging and—most importantly—a diagnostic injection. If numbing the joint relieves your pain, SI fusion is more likely to help.
Which approach is better: lateral or posterior?
Neither is “better” for everyone. Lateral gives broad, transfixing stability with 2–3 implants. Posterior is ideal when lateral access is limited or when posterior anatomy favors a direct dorsal fusion. We pick the safest, most effective route for your pelvis.
Will I need a brace?
Sometimes a short period of Bracing is used for comfort. We aim to wean quickly as your core and hips strengthen.
How long will the implants last?
They’re designed to be permanent. Over months, bone grows through/around them to complete the fusion.
What if I have back pain and hip pain too?
It’s common. We’ll sort out contributions from the lumbar spine, SI joint, and hip and treat each appropriately. When needed, we coordinate care across specialties.
Could I still need lumbar surgery later?
Possibly—if a separate lumbar issue progresses. That’s why we confirm the SI joint as the main pain generator before fusion.
Is this covered by insurance?
Often yes when criteria are met (failed conservative care, positive exam, diagnostic injection response). We’ll help navigate the details.




Dr. David L. Greenwald, MD
Neuro-Spine Surgeon

Call Now!
Desert Spine and Pain
A Spine Specialist is standing by.
Relief is just a phone call away!
Available Around the Clock.
Phone: (602) 566-9500
Email: [email protected]
Contact Us

Book a Consultation.
If you’re experiencing persistent lower back, hip, or pelvic pain that hasn’t responded to conservative care, Sacroiliac Joint Fusion—either minimally invasive posterior or lateral—may be the solution. Dr. Greenwald and his compassionate team will conduct a thorough evaluation, review imaging, and determine which approach is best suited for your condition. Every step you take toward expert spine care brings you closer to comfort, strength, and freedom of movement. Schedule your consultation today and learn how Dr. Greenwald’s minimally invasive SI joint fusion techniques can help you return to an active, pain-free life.
Voted Best Spine Doctor
Over 30 Years Experience in Orthopedic & Neuro Spine Surgeries.

Dr. David L. Greenwald, M.D., F.A.C.S.
Neurosurgeon | Spine Surgeon | Regenerative Medicine
Dr. David L. Greenwald, MD, FACS, is a board-certified spine surgeon with advanced expertise in Sacroiliac (SI) Joint Fusion, including minimally invasive posterior and lateral approaches. This procedure is designed to stabilize the SI joint, which connects the spine to the pelvis, and relieve chronic pain caused by joint degeneration, instability, or injury. Using state-of-the-art imaging and small incisions, Dr. Greenwald precisely places specialized implants to fuse the joint and restore alignment while minimizing muscle disruption and recovery time. His patient-centered, minimally invasive techniques have helped individuals throughout South Florida achieve long-term pain relief, improved stability, and restored quality of life.
Book your Spine Care Consultation Today!


Desert Spine and Pain
Patient Centered & Partner Focused
Quick Links
Resources
Connect With Us
© Desert Spine and Pain. 2026. All Rights Reserved. Sitemap















