Fusion
Cervical Fusion (Anterior or Posterior)
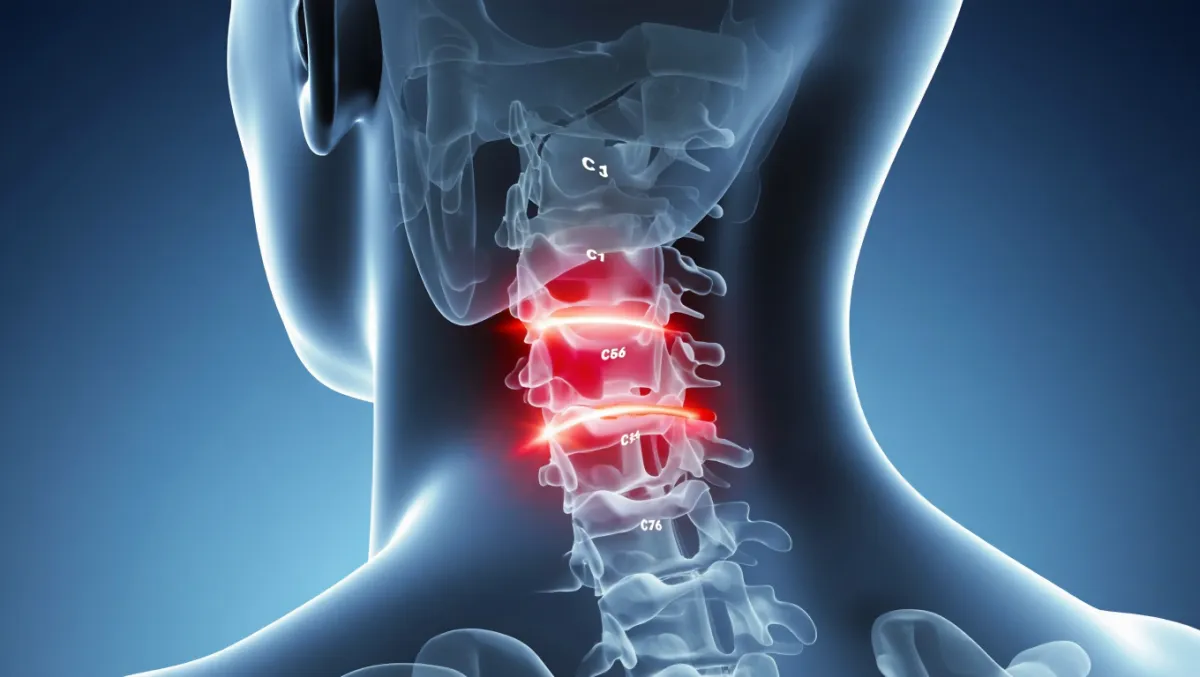
Stabilizing the Neck and Relieving Nerve or Cord Compression
Cervical fusion is a surgical procedure that joins two or more vertebrae in the neck to stop painful or unstable motion. It can be performed through the front of the neck (anterior approach) or the back of the neck (posterior approach). At Desert Spine and Pain, neurosurgeon Dr. David L. Greenwald, M.D., FAANS, FACS performs both anterior and posterior cervical fusions, selecting the safest and most effective approach for each patient’s unique condition.

Over 100 5-Star Reviews!

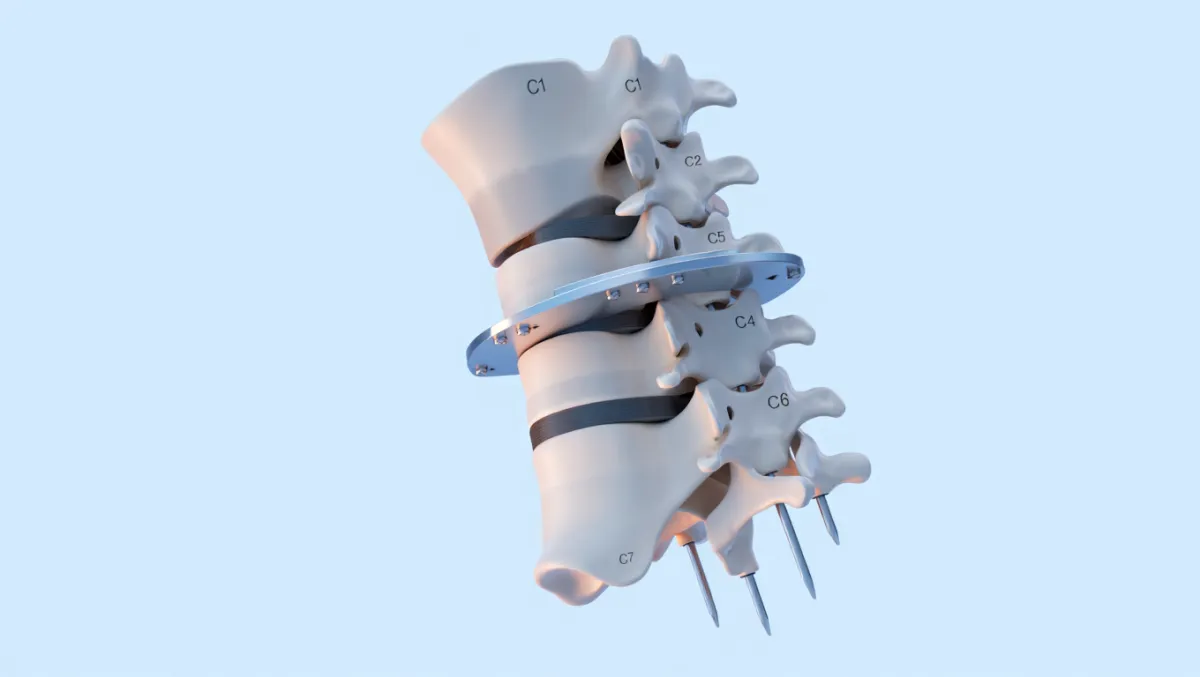
What Is Cervical Fusion?
In simple terms: We remove the damaged disc or bone causing nerve compression and fuse the affected vertebrae together with a bone graft and implants for long-term stability.
Scientifically: Cervical fusion involves decompression of neural elements, placement of an interbody graft or bone blocks, and rigid fixation (plate, rods, or screws) to promote arthrodesis through osteogenesis and immobilization of the motion segment.
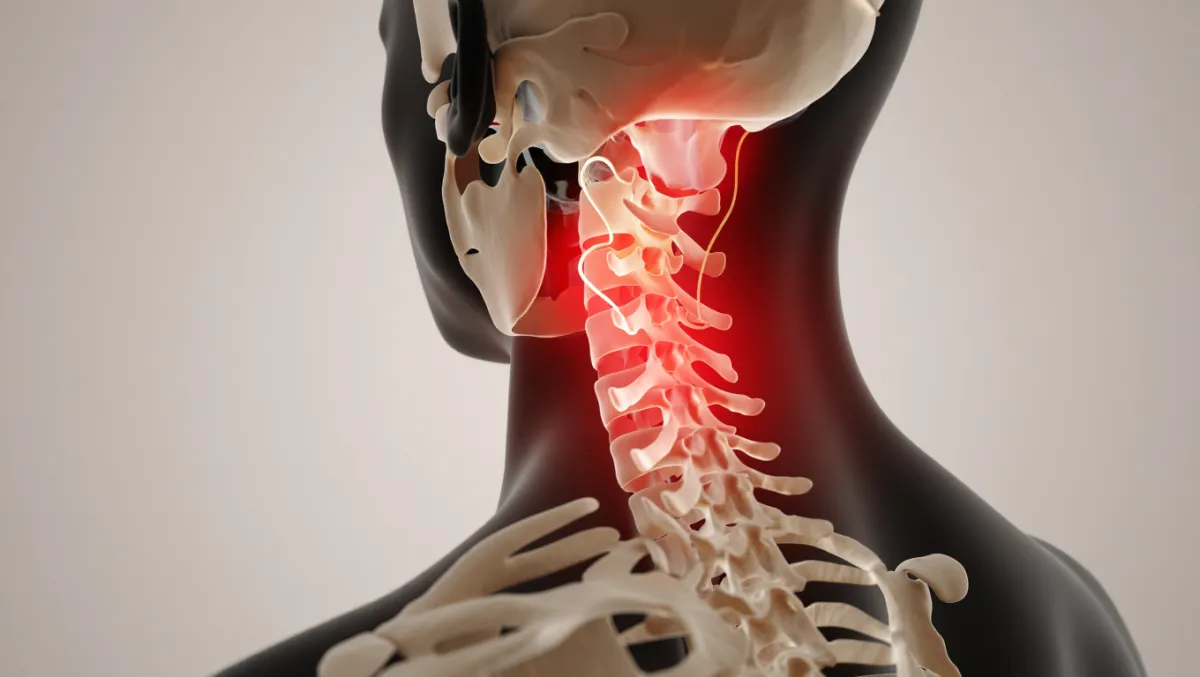
Conditions Treated
Herniated cervical discs
Cervical radiculopathy (arm pain, numbness, weakness)
Cervical myelopathy (spinal cord compression)
Degenerative disc disease in the neck
Spinal deformity or instability
Trauma and fractures of the cervical spine
Types of Cervical Fusion
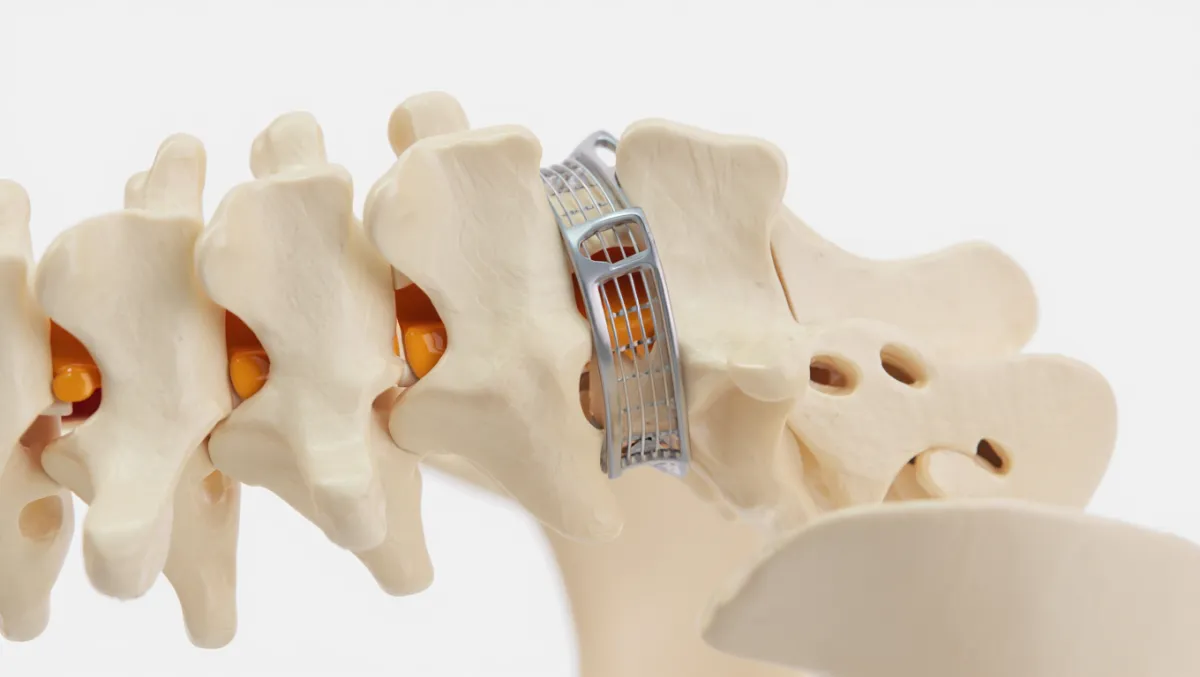
Anterior Cervical Fusion (ACDF)
Small incision in the front of the neck
Disc removed, nerve roots and spinal cord decompressed
Bone graft/cage placed, secured with a titanium plate
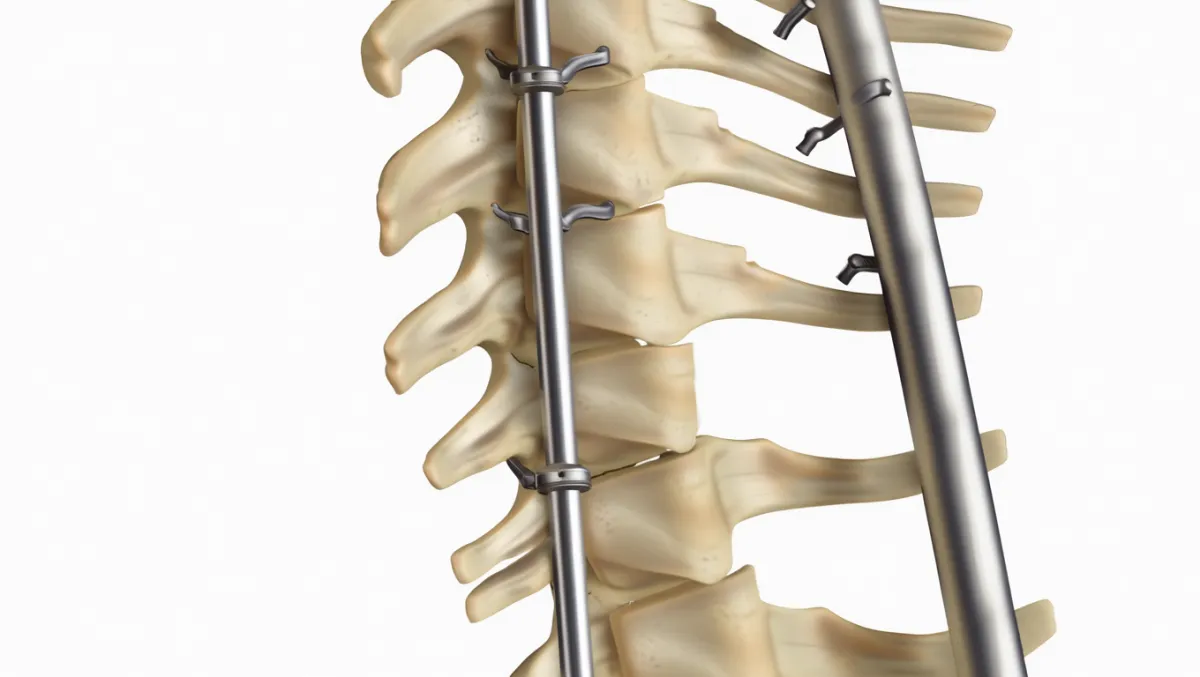
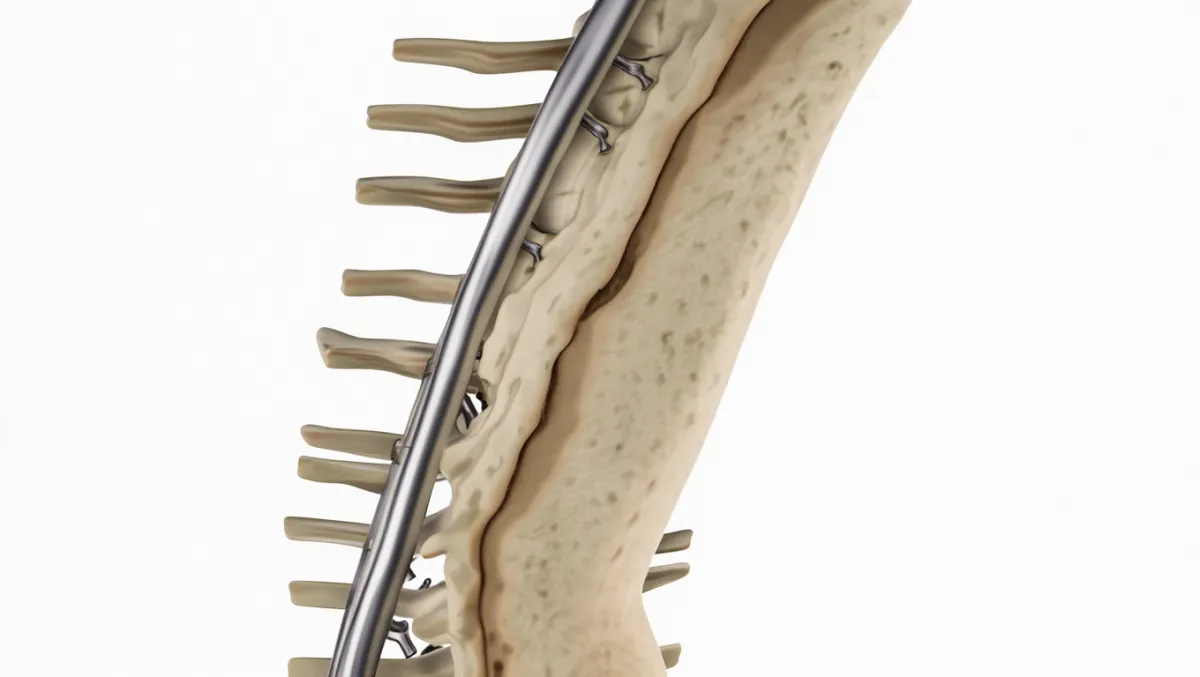
Posterior Cervical Fusion
Incision made in the back of the neck
Bone graft placed along posterior elements (lamina, lateral masses)
Screws and rods provide rigid stabilization
Used for multi-level disease, deformity, or when anterior approach isn’t ideal
The Cervical Fusion Procedure: Step by Step
Plain-English Overview
Anesthesia: You’re asleep under general anesthesia.
Incision: Either front (anterior) or back (posterior) depending on condition.
Disc/lamina removal: Damaged disc or bone spurs removed if needed.
Bone graft placement: Graft or cage inserted to promote fusion.
Implants: Plate (anterior) or rods/screws (posterior) stabilize the spine.
Closure: Small incision closed; patients often walk the same or next day.
Surgeon-Level Detail
Anterior approach: Smith-Robinson exposure; microsurgical discectomy; PLL resection; interbody cage with graft; anterior plate fixation.
Posterior approach: Midline incision; subperiosteal dissection; lateral mass or pedicle screw placement; decortication; autograft/allograft placement over lamina/facets; rods secured.
Fusion biology: Autograft (iliac crest), allograft, or synthetic substitutes enhance arthrodesis.
Benefits
Provides long-term stability for unstable or degenerative conditions
Relieves nerve and spinal cord compression
Restores alignment and posture
High success rates with modern implants and biologics
Choice of anterior vs. posterior allows tailored approach
Risks & Limitations
Infection, bleeding, anesthesia risks
Difficulty swallowing or hoarseness (anterior)
Muscle soreness or stiffness (posterior)
Non-union (pseudoarthrosis), especially in smokers
Adjacent segment degeneration over time
Recovery Timeline
Day 0–1: Walk the same or next day; short hospital stay for most
Weeks 1–2: Mild soreness; swallowing difficulty possible after anterior fusion
Weeks 2–6: Desk work and light activity resumed
6–12 weeks: Structured physical therapy; fusion consolidating
3–6 months: Return to most activities
6–12 months: Fusion confirmed on X-rays; full recovery reached
Why Choose Desert Spine and Pain?
Expert neurosurgeon: Dr. Greenwald specializes in both anterior and posterior cervical fusion techniques
Comprehensive approach: Careful evaluation to choose the safest, most effective route
Advanced technology: Navigation, neuromonitoring, and microsurgical tools ensure precision
Patient-first philosophy: We focus on conservative care first and guide patients through every step of recovery
Frequently Asked Questions
How do I know if I need anterior or posterior fusion?
The choice depends on your condition. Anterior is best for disc disease and nerve compression in front of the cord; posterior is used for multi-level disease, deformity, or instability.
Will fusion limit my neck motion?
Yes, at the fused level—but most patients notice little difference unless multiple levels are fused.
How long before I feel relief?
Arm pain often improves immediately; neck pain takes longer as tissues heal.
Do I need a brace after cervical fusion?
Sometimes. We may recommend a collar short-term depending on stability and bone quality.
How does Desert Spine and Pain perform cervical fusion differently?
We offer both anterior and posterior approaches, tailoring the plan to your anatomy and condition for the safest, most effective result.




Dr. David L. Greenwald, MD
Neuro-Spine Surgeon

Call Now!
Desert Spine and Pain
A Spine Specialist is standing by.
Relief is just a phone call away!
Available Around the Clock.
Phone: (602) 566-9500
Email: [email protected]
Contact Us

Book a Consultation.
If you’re experiencing chronic neck pain, numbness, or weakness due to cervical spine disease, Cervical Fusion Surgery may provide the lasting relief you need. Dr. Greenwald and his compassionate team will perform a detailed evaluation, explain whether an anterior or posterior approach is best for your case, and guide you through every step of your recovery. Every step you take toward advanced spine care brings you closer to strength, stability, and restored quality of life. Schedule your consultation today and discover how Dr. Greenwald’s expertise in cervical fusion can help you move and live without pain.
Voted Best Spine Doctor
Over 30 Years Experience in Orthopedic & Neuro Spine Surgeries.

Dr. David L. Greenwald, M.D., F.A.C.S.
Neurosurgeon | Spine Surgeon | Regenerative Medicine
Dr. David L. Greenwald, MD, FACS, is a board-certified spine surgeon with advanced expertise in Cervical Fusion Surgery, performed through either an anterior (front) or posterior (back) approach to the neck. This procedure is designed to stabilize the cervical spine, relieve nerve or spinal cord compression, and treat conditions such as herniated discs, degenerative disc disease, spinal stenosis, or instability. Dr. Greenwald carefully determines the best surgical approach based on each patient’s condition and anatomy, using advanced imaging and minimally invasive techniques to ensure precision and promote faster recovery. His expertise and patient-first approach have helped countless individuals throughout South Florida regain comfort, mobility, and long-term spinal stability.
Book your Spine Care Consultation Today!


Desert Spine and Pain
Patient Centered & Partner Focused
Quick Links
Resources
Connect With Us
© Desert Spine and Pain. 2026. All Rights Reserved. Sitemap















